Center for Human Nutrition
Zvitambo – Zimbabwe
History of the Site
Establishing the site

- The Zvitambo Institute for Maternal and Child Research was established in 1996; it's name makes use of the Shona word zvitambo, which indicates both a healthy baby and a full-bodied young woman.
- Zvitambo's initial aim was to serve as an African site for a small-scale replication and safety trial, building on findings from Indonesia that had indicated neonatal Vitamin A supplementation was both safe and could improve mortality in young infants.
- Research at the site ultimately informed science and policy regarding the importance of exclusive breastfeeding in preventing mother-to-child-transmission of HIV and the need for transformative approaches to WASH.
- Zvitambo has established long-lasting connections with the University of Zimbabwe, the Harare City Health Department, and the Medical Research Council of Zimbabwe. The Institute is now a completely independent entity from Johns Hopkins University.
Seminal Research
Research list and links

- The Institute's initial work focused on investigating the efficacy of Vitamin A in reducing neonatal mortality and mother-to-child transmission of HIV as well as in speeding healing after labor and delivery. The findings from this work indicated:
- Neither postpartum maternal nor neonatal vitamin A supplementation reduced infant mortality among HIV-negative women with adequate vitamin A status. [Link]
- In HIV-positive women, neither maternal nor neonatal vitamin A supplementation affected mother-to-child transmission of HIV or neonatal survival; however, infants who had seroconverted after six weeks of life saw a 28-percent decline in mortality when supplemented. Conversely, infants who remained HIV-negative at six-weeks saw two-fold higher rates of mortality following supplementation. [Link]
- Exclusive breastfeeding substantially reduced post-natal HIV transmission from HIV-positive mothers to their HIV-negative infants. [Link]
- Timing of maternal-infant HIV transmission (whether the infant was non-infected, infected in-utero, intrapartum, or postnatally) was strongly predictive of neonatal mortality and time to death when compared to HIV-negative children of HIV-negative mothers. [Link]

- Subsequent work, as part of the SHINE trial, focused on the hypothesis that stunting in children living in conditions of poor water, sanitation, and hygiene (WASH) could be reduced with household-level WASH interventions, additive to the benefits of improved infant feeding. The findings from this work indicated:
- Neither infant and child feeding nor household-level WASH interventions (improved pit latrines, hand-washing stations, liquid soap, point-of-use water chlorination, and clean play spaces) prevented enteric infections in young children. [Link]
- While infant feeding improved length-for-age Z scores, WASH programming had no impact on stunting. Previous observational studies that had linked household WASH interventions with decreases in diarrhea had all relied on daily to fortnightly interactions between families and health promoters. Existing, routine WASH approaches cannot approach such frequency and are insufficient to reduce environmental fecal contamination or have an impact on child growth. [Link]
- HIV-exposed children who received the feeding intervention had lower rates of stunting and anemia but did not show any benefit from WASH interventions. [Link]
Ongoing Studies
Integrated Maternal Calcium + Aspirin + Multiple Micronutrients (CAMMS) During Pregnancy
PI: Dr. Jean Humphrey
Duration: September 2023 - April 2025
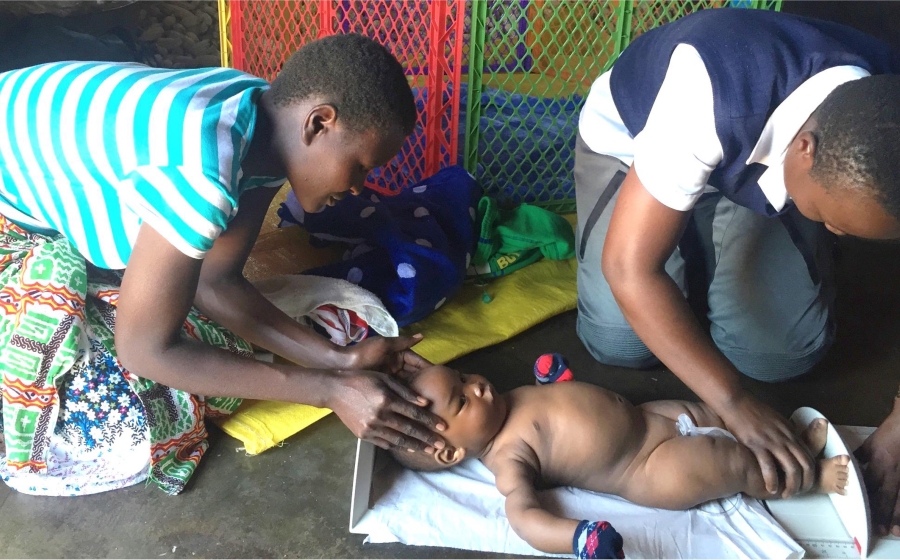
- Objectives: Pre-term birth, small-for-gestational age, and stillbirth affect millions of infants globally, predominately in Sub-Saharan Africa and Southeast Asia, and contribute to high rates of neonatal death, childhood stunting, and later life morbidities. Three evidence-based, low-cost, safe prenatal interventions can help prevent these adverse birth outcomes: calcium, aspiring, and multiple micronutrient supplements. Moreover, each has distinct biologic mechanisms of action that address different pregnancy complications; this suggests that combining them may have additive impact. The CAMMS trial is an individually randomized, unblinded, phase III trial comparing these three interventions to the standard of care, iron-folic acid supplementation, during pregnancy. The primary outcome is the proportion of infants with preterm birth, and birthweight, gestational age at delivery, and weight-for-gestational-age and maternal preeclampsia are secondary outcomes.
- Participants: 12,000 pregnant women in Zimbabwe, Burkina Faso, and Pakistan
- Donors: Bill and Melinda Gates Foundation
- Collaborators: Aga Khan University, Karachi, Pakistan; Institut Africain de Santé Publique, Ouagadougou, Burkina Faso; Cristiana Health Care, Newark, DE; Columbia University, New York, NY.
