The Other Pandemic: Why TB Deserves Your Attention
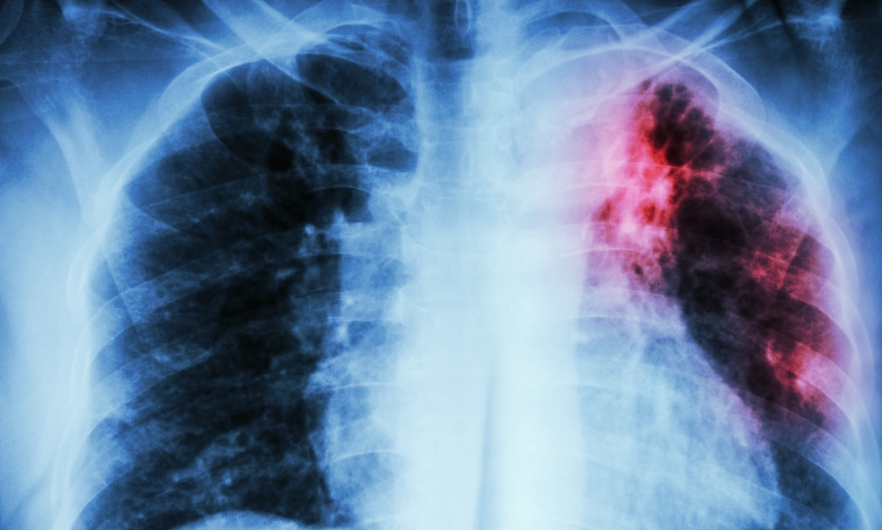
Before COVID-19, another pandemic disease was killing nearly 1.5 million people a year, for decades, but attracting nowhere near the attention: tuberculosis.
TB is preventable and curable—yet it is the world’s second-deadliest infectious disease (behind COVID-19).
- An estimated 1.8 billion people—about a quarter of the world’s population—are infected with Mycobacterium tuberculosis, the bacterium that causes TB.
- Up to 10% of them will become ill with active TB in their lifetime, enabling them to infect others.
- In 2019, an estimated 3 million of the 10 million people who fell ill with TB were never diagnosed.
- The demands of the coronavirus pandemic have reversed years of progress in reducing TB’s death toll—with deaths increasing in 2020 for the first time in over a decade.
TB disease mainly impacts the lungs, but it can attack any part of the body, such as the kidneys, spine, and brain—and can be fatal if left untreated.
TB bacteria become airborne when an infected person coughs, sneezes, or even speaks. The disease usually spreads during prolonged exposure with everyday contacts, like family members and colleagues. And conditions of poverty, such as malnutrition and overcrowded, poorly ventilated living spaces, create ideal settings for TB to spread.
Ninety-five percent of the global TB burden falls on developing countries—but this is a disease that should be on everyone’s radar, says Amesh Adalja, senior scholar at the Johns Hopkins Center for Health Security.
As COVID-19 has made clear, “infectious disease uncontrolled in one part of the world affects people everywhere,” bringing with it not only the disease itself, but the cascading effects on human health and productivity. TB alone could cost the global economy $1 trillion by 2030—but funding to fight TB is on the decline.
And as with COVID-19, the chances of fending off an infectious disease epidemic depend largely on the quality of diagnostics, treatments, and vaccines.
When it comes to TB, all three are falling short, explains Adalja.
Some innovations are paving a way forward, but clunky diagnostics, a century-old vaccine, and arduous treatments—as well as the rising toll of drug-resistant forms of the disease—all pose major challenges to WHO’s goal of stamping out TB by 2035, especially in the face of COVID-19.
TESTING FOR TB
“We’re playing a lot of catch up.”
While better TB diagnostics to improve surveillance are badly needed, funding has stagnated. Global funding for TB research reached $915 million in 2020, but that’s less than half the UN’s annual goal of $2 billion.
Currently, diagnosing active TB disease requires multiple tests—first to spot the bacteria, and additional tests to determine whether the infection has latent TB or TB disease.
The current go-to diagnostics—blood tests and skin tests—are “not easy,” says Adalja. For one, they can’t decipher whether a patient has an active or latent infection, and further tests like sputum samples and chest x-rays are required to diagnose active TB disease—a major hurdle in low-resource communities with limited health care infrastructure.
And the nature of someone’s TB can change. Even among those infections that are detected: “We've got this huge burden of people with latent tuberculosis, but we don't know which ones are going to convert over to active tuberculosis,” says Adalja.
Rapid molecular tests now recommended by the WHO offer a promising alternative. These tests can diagnose TB, and spot whether it is drug-resistant, in less than 2 hours without the need for high-tech labs or high-skilled personnel.
They could be a game-changer for improving TB surveillance so that patients can get the treatment they need. Last year, WHO took a step in that direction, issuing new recommendations that encourage member states to expand the rollout of new classes of rapid molecular tests for TB and drug-resistant TB. These rapid tests may be the wave of the future, but they are relatively new and costlier than other forms of testing, and their availability is still limited.
“There has been a concerted effort to use molecular diagnostics and there are some that are available, but it's still something that I think we're playing a lot of catch up and there's a lot of unrecognized tuberculosis in the world,” says Adalja.
And that includes in the U.S. Even though the country is “at the nadir of cases,” clocking less than 8,000 in 2021, Adalja believes many cases are being missed, particularly among vulnerable communities such as people with HIV and diabetes, and newcomers to the US from high-incidence countries.
“I think there needs to be a lot of education to make sure that patients are linked with primary care providers that have the resources to be able to deal with tuberculosis.”
TREATING TB
“It's not just taking a five-day course of antibiotics.”
Treating tuberculosis can take anywhere from six months to over two years for drug-resistant infections, and involves at least four different antibiotics that must be taken exactly as prescribed even when patients start to feel better, usually after a few weeks.
When patients stop taking the drugs before their body has completely kicked the disease, surviving bacteria can adapt and become resistant to existing drugs. In fact, about a third of deaths caused by antimicrobial infections today are due to drug-resistant TB.
The drugs required to treat drug-resistant TB are highly toxic, can cost well over $20,000—compared to a few hundred for non-drug-resistant TB. Treatment can require months of injections, IV infusions, and some 14,000 pills.
A relatively new drug regimen could be a game-changer, offering a six-month, all-oral treatment for multidrug-resistant TB; it’s FDA approved and this year WHO updated its TB treatment guidelines to include it. But at $800 per treatment, cost is still a major barrier to access in TB-endemic countries.
Limited treatment options are particularly worrisome for people who have HIV—who are 18 times more likely to develop active TB than those without the virus.
The weakened immune systems of those with HIV—especially if it’s untreated—allow TB to thrive, requiring an even more complex cocktail of treatments that are challenging to manage.
“You have to deal with both issues at the same time, because they're feeding off of each other,” Adalja says.
MODERNIZING TB VACCINES
“The current vaccine is just not that good.”
The Bacillus Calmette-Guérin vaccine, or BCG, is the only licensed TB vaccine. It’s over 100 years old, and doesn’t do much to prevent TB transmission, says Adalja.
First administered for TB in 1921, BCG is essentially unchanged from its original formula.
The shot is given to some 100 million children every year and does a good job protecting them against serious childhood forms of TB. But crucially, it doesn’t prevent TB in the lungs of adults, the key driver of TB transmission.
But the stunning speed and success of mRNA COVID-19 vaccines may pay dividends in the search for a better TB jab. A number of research groups worldwide are working on mRNA vaccines for TB, and clinical trials will begin this year for a formula developed by BioNTech and the Bill & Melinda Gates Foundation.
So, while the COVID-19 pandemic has overshadowed tuberculosis, diverting attention and resources from TB and other health priorities, it has spurred an unprecedented innovation and awareness of interconnected health crises.
“The world is aware of infectious disease now in a way that they haven't been probably for decades and decades,” says Adalja.
“It improves everybody's life when you control infectious diseases anywhere in the world. The more humans are thriving, the better it is for all the others.”
Annalies Winny is Associate Editor of Global Health NOW.
RELATED:
- How COVID-19 Set Back India’s Battle with Leprosy
- Covid-19 Hinders Pakistan's Progress on Cutaneous Leishmaniasis





