An Update on Omicron Subvariants
With five versions of omicron circulating, vaccines are working against severe disease, not against infection.
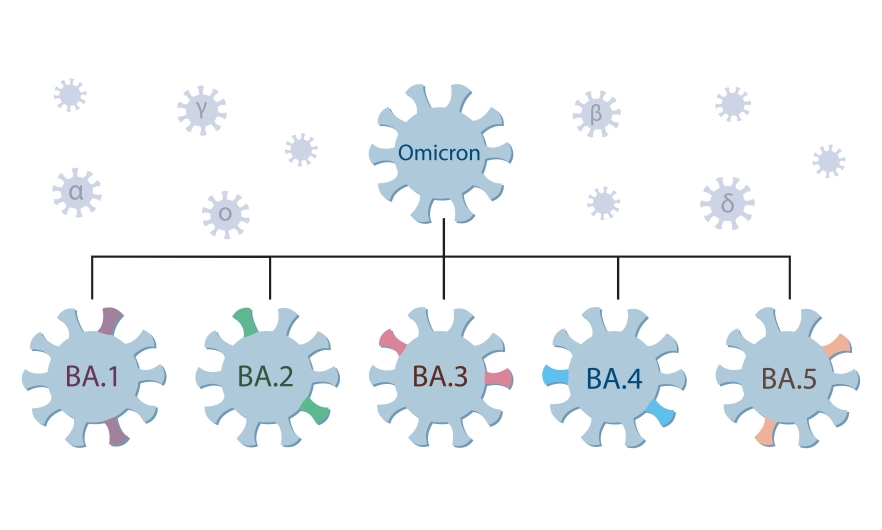
Omicron is mutating in giant leaps, with scientists racing to keep up. Its diversity is challenging vaccine efficacy and complicating treatment. But this fall, broad spectrum bivalent vaccines may help mitigate the seemingly never ending spread of COVID-19.
In this Q&A, adapted from the June 6 episode of Public Health On Call, Stephanie Desmon talks with virologist Andy Pekosz, PhD, a professor in Molecular Microbiology and Immunology, about the diverse range of omicron subvariants, omicron-specific vaccines, and what we can expect to see in the future from this “game-changer” variant.
What’s happening now with omicron’s subvariants?
When a variant emerges, it never stops mutating and changing. And omicron, being a really transmissible virus, amplified how quickly we see these mutations emerge. We went from one version to five [in a relatively short period of time].
Each of these [subvariants] are different from each other. Some scientists say that what we call omicron subvariants now are equivalent to what we referred to as different variants earlier in the pandemic. There's a lot of diversity in omicron, which is contributing to issues with COVID-19 vaccine efficacy and treatments.
How are these subvariants impacting vaccine efficacy and treatments?
First, all these omicron variants are good at evading some portion of the vaccine-induced immunity. Vaccines are still protecting against severe disease, but even if you are vaccinated, if you're exposed, you should expect to have a symptomatic infection. We're seeing case numbers go up, but we're not seeing hospitalizations, disease severity, or death go up anywhere close to that same rate. Vaccines are working against severe disease, not against infection.
The other important thing is that these variants of omicron have different susceptibilities to different monoclonal antibody treatments. It becomes tricky to figure out which treatment you can take. We don't have the capability to quickly tell someone, “You're infected with BA.4,” yet the efficacy of the treatment is completely dependent upon which variant you're being infected with.
Are new variants making it easier to become reinfected?
This family of omicron subvariants transmit more effectively than any other variant we've seen so far. They evade a large portion of the vaccine induced immunity; you're protected from the severe disease, but can get infected.
Omicron was a complete game-changer when it emerged. It had such unique properties, that it pushed the COVID-19 pandemic into a completely different area that is similar to what we deal with with seasonal influenza. We're now completely focused on making sure that we're doing enough to protect the vulnerable people in the population. Relatively healthy individuals will use vaccines to try to limit spread, but they’re not going to protect people from infection as well as we hoped when the vaccines were initially rolled out.
Why is omicron evolving so quickly?
There are a lot of theories out there. Some theories suggest that people who have slightly compromised immune systems are generating some of these variants over time.
We really don't understand where this happens. With seasonal flu, we see one or two mutations occur that change the virus, that makes us update vaccines—but it's at a steady rate. What we see with SARS-CoV-2, is that these variants emerge with lots of mutations—making leaps when they change. They’re not moving in small steps. Understanding that is going to be critical to fine-tuning our strategies to be as effective as possible in terms of limiting SARS CoV-2 spread and evolution in the future.
Would a virus that doesn't mutate so quickly be gone by now?
It would be present at a very low level. If a virus can't evade immune responses, then the number of people that are susceptible to it shrinks each year. Often, the virus then becomes focused in either younger populations who haven't been exposed, or older populations, whose immunity is waning and can't respond as quickly to an infection.
We're not seeing that with SARS-CoV-2. We're seeing that the virus is changing and still infecting healthy individuals. Understanding why that's happening is going to be crucial to dealing with COVID-19 as an annual disease.
Are omicron vaccines coming soon?
It looks like that’s what's going to happen in the fall of this year. There's been good data published by Moderna and Pfizer showing that new formulations combining omicron with other variants can give a broader immune response that recognises omicron and older variants more efficiently.
That's really important, because omicron is so distinct from older variants. You want a vaccine that covers both bases. If you get too specific to omicron, you run the risk of having the virus change and another variant emerging.
These are called bivalent vaccines. While they haven't been authorized yet by the FDA, there is a lot of data suggesting that these bivalent vaccines are going to be recommended for at least vulnerable people in the population, and for virtually everyone as a booster.
Should people who haven’t gotten their second booster wait for this new formulation in September?
It's always important to balance risk with potential benefit. [If you’re healthy,] I think it's good to wait for these bivalent vaccines, because they potentially provide greater protection against infection and severe disease. But if you're in a high risk population, for example, over 70 and on immunosuppressive therapies, you shouldn't wait. When you become eligible for the booster, you want to get it—it's important in high risk populations to maintain strong immunity. You don't want to wait, let your immune system run down, and run the risk of getting an infection.
are these new vaccines how we knock out OMICRON?
We're getting better at inducing the broad immunity that keeps variants from emerging. We'll never eliminate COVID-19 from the human population, now that it's been established.
I think that this next generation of bivalent vaccines is showing us a path to get vaccines that are broad in terms of their protection, but that may have the potential to protect you for longer periods of time, so that you can have a higher level of confidence that when you get the vaccine, you'll be protected not only from severe disease but also from infection.
Could an unvaccinated person start their immunizations with the new vaccine?
Absolutely. There are a lot of people who got omicron infections who weren't vaccinated. It's becoming clear that omicron by itself doesn't induce a really strong immune response like previous variants did.
Even that portion of the population that didn't want to get vaccinated, or who got omicron need to be told, “now you need to get the booster to really make sure that you're protected from a reinfection going forward.” Omicron infection by itself isn't going to be enough to protect people from reinfection for the long term.
Is the fact that so many vaccinated people are still getting COVID going to hurt vaccination efforts going forward?
We struggle with this with seasonal influenza vaccines. All of us in the scientific community want the best vaccine possible. No scientists like to say, “well, it protects against severe disease but not from infection.” We realize that that's not what people want.
I do feel like we're moving forward with the realization in the scientific community, and in the pharmaceutical community, that we need to make better vaccines that are more than just protecting from severe disease. This bivalent vaccine, that's coming in the fall, is a good step in that direction. Scientists and pharmaceutical companies need to do better at trying to come up with more effective COVID-19 vaccines. We know SARS-CoV-2 is going to be here and we're not going to get rid of it from the human population. But, we now have to continue our research efforts to make sure that we're improving those vaccines and getting them to a better level of inducing strong and long term immunity.
Stephanie Desmon is the co-host of the Public Health On Call podcast. She is the director of public relations and marketing for the Johns Hopkins Center for Communication Programs, the largest center at the Johns Hopkins Bloomberg School of Public Health.
Want COVID-19 articles like these in your inbox? Subscribe to Expert Insights, a 2x-per-week newsletter with the latest insights and research from public health experts.





