Can a Mask Protect Me? Putting Homemade Masks in the Hierarchy of Controls
Covid 19 interview: Are face masks necessary?
Mary Doyle, MPH, RN, COHN-S/CM
Environmental Health and Engineering Johns Hopkins Bloomberg School of Public Health
Kirsten Koehler, PhD
Associate Professor Environmental Health and Engineering Johns Hopkins Bloomberg School of Public Health
Ana Rule, PhD
Assistant Professor Environmental Health and Engineering Johns Hopkins Bloomberg School of Public Health
BY KIRSTEN KOEHLER AND ANA RULE | April 2, 2020
Kirsten Koehler, PhD
Associate Professor
Environmental Health and Engineering
Johns Hopkins Bloomberg School of Public Health
Ana Rule, PhD
Assistant Professor
Environmental Health and Engineering
Johns Hopkins Bloomberg School of Public Health
There has been a lot of talk over the last week about the use of masks. What kind of masks are available, who needs them, and can they be reused?1-3 However, the public wants to know if they should make masks at home and if they should be wearing them in public. These masks are typically made out of different types of cloth found in the home. As aerosol scientists and occupational health professionals, we think about this question differently. It starts with the hierarchy of controls – a framework used in occupational health to protect workers with the most effective controls. The framework, shown in Figure 1, is an upside-down pyramid, showing five levels of control efforts: elimination, substitution, engineering controls, administrative controls, and personal protective equipment or PPE. They are ranked in order of effectiveness to prevent hazardous exposures and disease. The framework also applies well for controlling exposures to novel coronavirus.
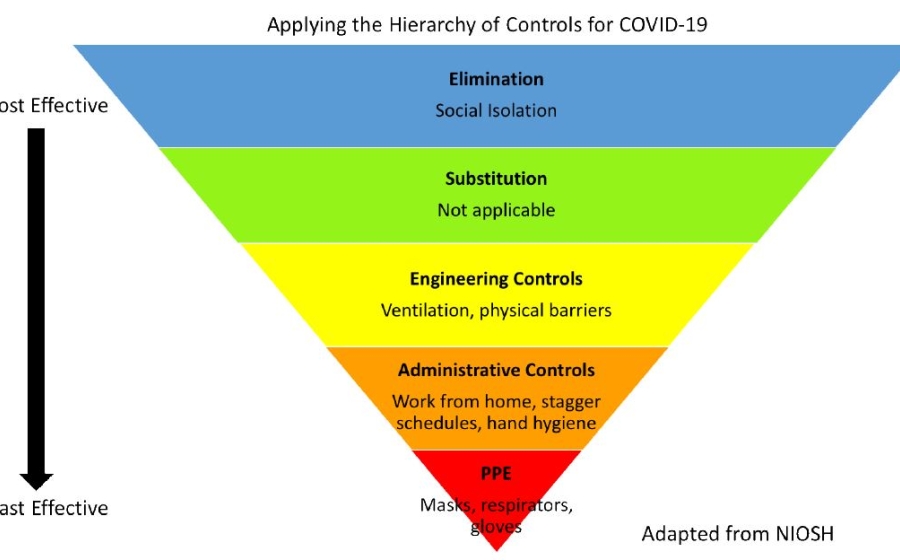
Figure 1: Applying the Hierarchy of Controls for COVID-19. Adapted from the CDC website.
The most effective means to prevent exposures to COVID-19 is through elimination – physically removing the hazard (COVID-19). For workplaces deemed necessary, such as hospitals, supermarkets, and banks, this means making sure workers are not coming in when they are ill or have potentially been exposed to others who are ill. In this way, we can eliminate (to the best of our ability) the means of transmission among the workers. For the general public, this means eliminating unnecessary trips to the store or other places where you could come in contact with infected individuals and keeping your distance (6 ft)4 from other people when you must be away from your home. It also means staying home if you are sick or suspect that you have been around someone who is sick. Social isolation is one of our best tools to reduce the spread of infection. Social isolation is especially important in the context of COVID-19 because many individuals are asymptomatic and can, unknowingly, spread the virus any time they leave their home.
The next level is substitution – replacing a hazardous exposure with something less hazardous. In the case of COVID-19, this is not applicable.
The next level is engineering controls – separating the workers from the hazard. This is achieved in hospitals with a high ventilation rate that removes the air from a room where virus may be found. Some companies are installing extra barriers between workers and consumers. In homes, individuals may choose to run filtered home HVAC systems or open windows to bring in fresh air regularly. You might also choose to run an air purifier.
The fourth level is administrative controls – changing the way work is performed. For workplaces this can mean instituting work from home policies for all non-essential personnel. Many cities and states have already implemented this control. For essential personnel and workplaces, it can mean reducing the number of workers on a shift and keeping workers further apart. Staggering work schedules so people don’t have to come in contact with their shift replacement can also help. Some companies have also implemented buying online with curbside pick-up. For individuals, there are many examples you can implement in your home:
- Enforcing home handwashing rules so that everyone washes their hands after coming in from outside and before and after all meals.
- Allowing mail to sit for several days before handling it and washing hands immediately after touching mail.
- Disinfecting the outside of grocery containers, placing reusable grocery bags away from other people for several days or wash immediately, and then washing your hands after putting away groceries.
- Daily disinfection of high touch surfaces in your home.
It is important not to underestimate the role these practices can have in reducing infection risk.
The final, and LEAST effective control strategy is Personal Protective Equipment (PPE) – protecting workers with masks, gloves and other equipment. It is tempting to use PPE as the first line of defense, because it is (typically) readily available and inexpensive, but in reality, PPE is the least effective strategy because it relies on adequate supplies and proper and continuous use, which is difficult to achieve. At hospitals where medical staff are required to come into close contact with infected patients, PPE use is critical. However, hospitals also use other measures spanning the full hierarchy of controls, today and always, to protect both workers and patients. It is most important that medical staff have the PPE they need to do their work as safely as possible.
The use of homemade masks has gained a lot of attention on social media to help individuals reduce their risk of exposure to COVID-19. This is because when we cough, sneeze, and even talk, we all emit droplets into the air—small drops of moisture from the upper respiratory system—of various sizes. These droplets may carry viruses like the one that causes COVID-19. But there are two important things to consider: 1) Can the homemade masks remove virus-containing droplets? and 2) Will the homemade masks be used correctly to limit virus exposure? Homemade masks may remove some virus-containing droplets, but cannot remove them to the extent that PPE can. Thus, using homemade masks will still expose people to some risk. Furthermore, the use of PPE without some training may reduce their effectiveness and may enhance risk if contaminated masks are not handled properly. Perhaps you’ve seen someone at the grocery store wearing gloves, but still touching their face and using their cellphone. The virus does not penetrate the skin, so if someone is still spreading the virus to their face and high touch surfaces, the gloves provided no benefit. The use of disposable goods like gloves can also lead to unnecessary environmental pollution. Incorrectly used homemade masks could spread virus when people touch the mask then their face or other surfaces. Using homemade masks could also give people a false sense of security making them more likely to go out than if they didn’t have a mask, while providing only limited protection. Homemade masks are not traditional PPE.
There are two reasons to use a mask: 1) to protect yourself from inhaling virus-containing particles; and 2) to limit the number of virus-containing particles exhaled by infected (but potentially asymptomatic) individuals. Homemade masks are unlikely to protect you from infection, but they may reduce the number of virus-containing droplets exhaled by infected people.
Understanding why homemade masks cannot provide adequate protection requires that we understand how droplets, often called particles or aerosols, behave. Particles behave very differently in air depending on their size. Particles can range in size from 0.01 to 100 micrometers – a huge range. They are all very small; the largest particles have a size similar to the diameter of a human hair. Yet the difference in behavior between big and small particles is dramatic. Most of the particles we emit when we breathe, talk, cough, or sneeze are in the size range of 0.3 – 10 micrometers.5-7 A smaller number of particles may be up to 100 micrometers. Less is known about the number of particles that are very small (0.05 micrometers); however, because these particles are too small to carry a virus, we can neglect these for our understanding COVID-19 transmission.
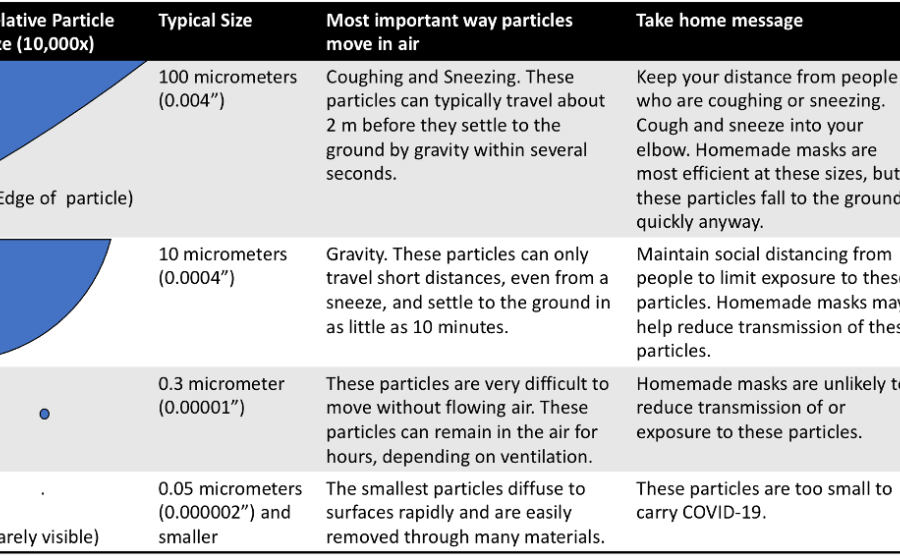
The very large particles (100 micrometers) are rapidly removed from the air by gravity – in just seconds. Keeping a 2-meter distance from anyone coughing and sneezing is likely sufficient to protect yourself from these particles. The 10 micrometer particles can typically travel only short distances from a cough or sneeze and settle to the ground in as little as 10 minutes. These particles may move through the room via air currents. Particles of this size can be removed with about 50-70% efficiency from homemade masks, depending on the material.8,9 However, the smaller particles, around 0.3 micrometers, are large enough to carry COVID-19, but are so small that gravity does not remove them from the air. These particles can stay in the air for hours, depending on the ventilation in the room. This size particle is the hardest for filters and masks to remove. For this reason, testing facilities use 0.3 micrometer particles to ensure the effectiveness of N95 masks (N95 means that the mask removes at least 95% of particles of this size). For homemade cloth masks, the removal efficiency of these particles will likely be around 20%.8
Although those making these homemade masks certainly have the best intentions to help reduce the COVID-19 pandemic, it is critical to understand their limitations. Reducing the number of virus-containing particles by 50% sounds like a big improvement, but this may not be adequate to ensure you don’t become infected. If you choose to wear a mask, do not assume you won’t get sick. Continue to practice social isolation (elimination control) and hand hygiene (administrative controls) as much as possible.
Here are a few frequently asked questions:
I know I have COVID-19, but I am not sick enough to be in a hospital. Should I wear a homemade mask?
Isolating yourself in a separate room as much as possible is likely to be most effective. Also, consider opening windows or using filtered HVAC systems to bring in fresh air. Remind your family members to wash their hands after every time they are near you. We recommend that anyone who knows or suspects they have COVID-19 use a homemade mask when they are around other people to limit the spread of the virus, if they do not have access to a surgical mask. This may reduce the risk of infection to family members and others close by.
I don’t think I have COVID-19, should I wear a homemade mask?
Some people who have COVID-19 do not have any symptoms and can spread the virus unknowingly. The best ways to prevent infection is to limit your exposure to other people through social/physical isolation, and practicing hand hygiene. Wearing a homemade mask may reduce the spread of virus to others via large droplets. However, it is unlikely that wearing a homemade mask will prevent you from becoming infected.
Is there a best homemade mask pattern?
There are many mask patterns on the internet and little is known about whether any specific type is better at removing particles than others. However, some materials are better at removing particles than others.9 Your mask should fit as snugly as possible around your face to limit airflow around the mask.
I have decided to wear a homemade mask, what are some best practices?
- Wash your hands with soap and water before you put on the mask.
- If your mask has ties, secure the bottom ties first with a bow around the nape of your neck. Then pull the mask by the upper ties over your mouth and chin and secure around your head.
- Wash your hands every time you touch your mask during the day! (Yes, every time.)
- Wash your mask every time you remove it and wash your hands with soap and water after removing the mask. Put the mask somewhere isolated until it can be washed.
- Assume that there could be virus on both sides of the mask any time you touch it.
- Wear a clean mask each time you need to put one on.
References
- Stanford Medicine. https://m.box.com/shared_item/https%3A%2F%2Fstanfordmedicine.box.com%2Fv%2Fcovid19-PPE-1-1?fbclid=IwAR0hBHV_Ad1tRryrLrVrwn-arlblWjL4aDqo02QkFIFWqBmqu21k36lcRC8. Published 2020. Accessed.
- Nebraska Medicine. https://www.nebraskamed.com/sites/default/files/documents/covid-19/n-95-decon-process.pdf. Published 2020. Accessed.
- Johns Hopkins Bloomberg School of Public Health. https://www.jhsph.edu/covid-19/articles/the-right-mask-for-the-task.html. Published 2020. Accessed.
- CDC. How to Protect Yourself. https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/prevention.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcoronavirus%2F2019-ncov%2Fprepare%2Fprevention.html. Published 2020. Accessed.
- Lindsley WG, Pearce TA, Hudnall JB, et al. Quantity and size distribution of cough-generated aerosol particles produced by influenza patients during and after illness. J Occup Environ Hyg. 2012;9(7):443-449.
- Papineni RS, Rosenthal FS. The Size Distribution of Droplets in the Exhaled Breath of Healthy Human Subjects. JOURNAL OF AEROSOL MEDICINE. 1997;10(2):105-11
- Chao CYH, Wan MP, L.Morawska, et al. Characterization of expiration air jets and droplet size distributionsimmediately at the mouth opening. Aerosol Science. 2009;40:122-133.
- Rengasamy S, Eimer B, Shaffer RE. Simple respiratory protection--evaluation of the filtration performance of cloth masks and common fabric materials against 20-1000 nm size particles. Ann Occup Hyg. 2010;54(7):789-79
- Davies A, Thompson K-A, Giri K, Kafatos G, Walker J, Bennett A. Testing the Efficacy of Homemade Masks: Would They Protect in an Influenza Pandemic? Disaster medicine and public health preparedness. 2013;7:413-418.
